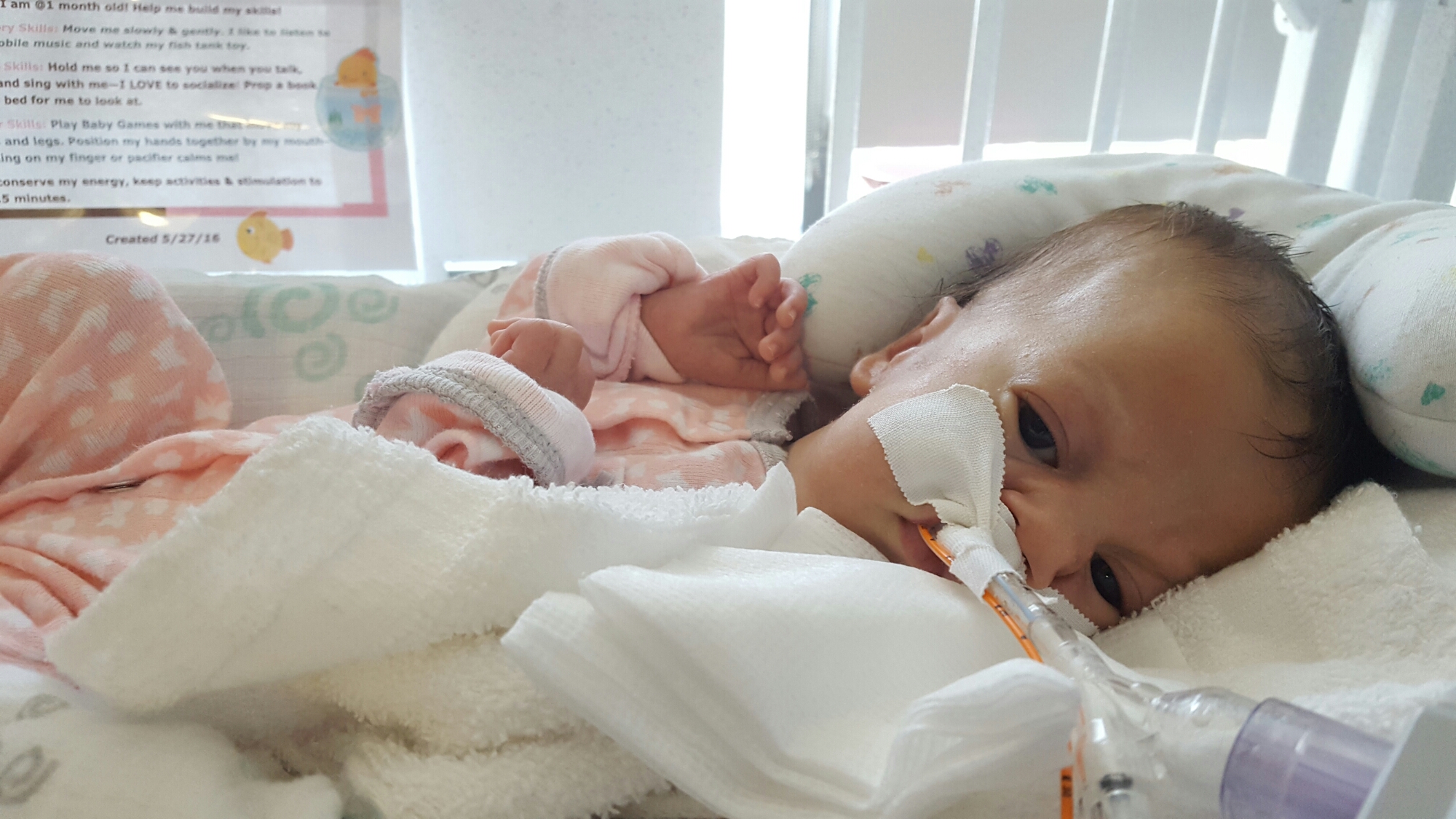
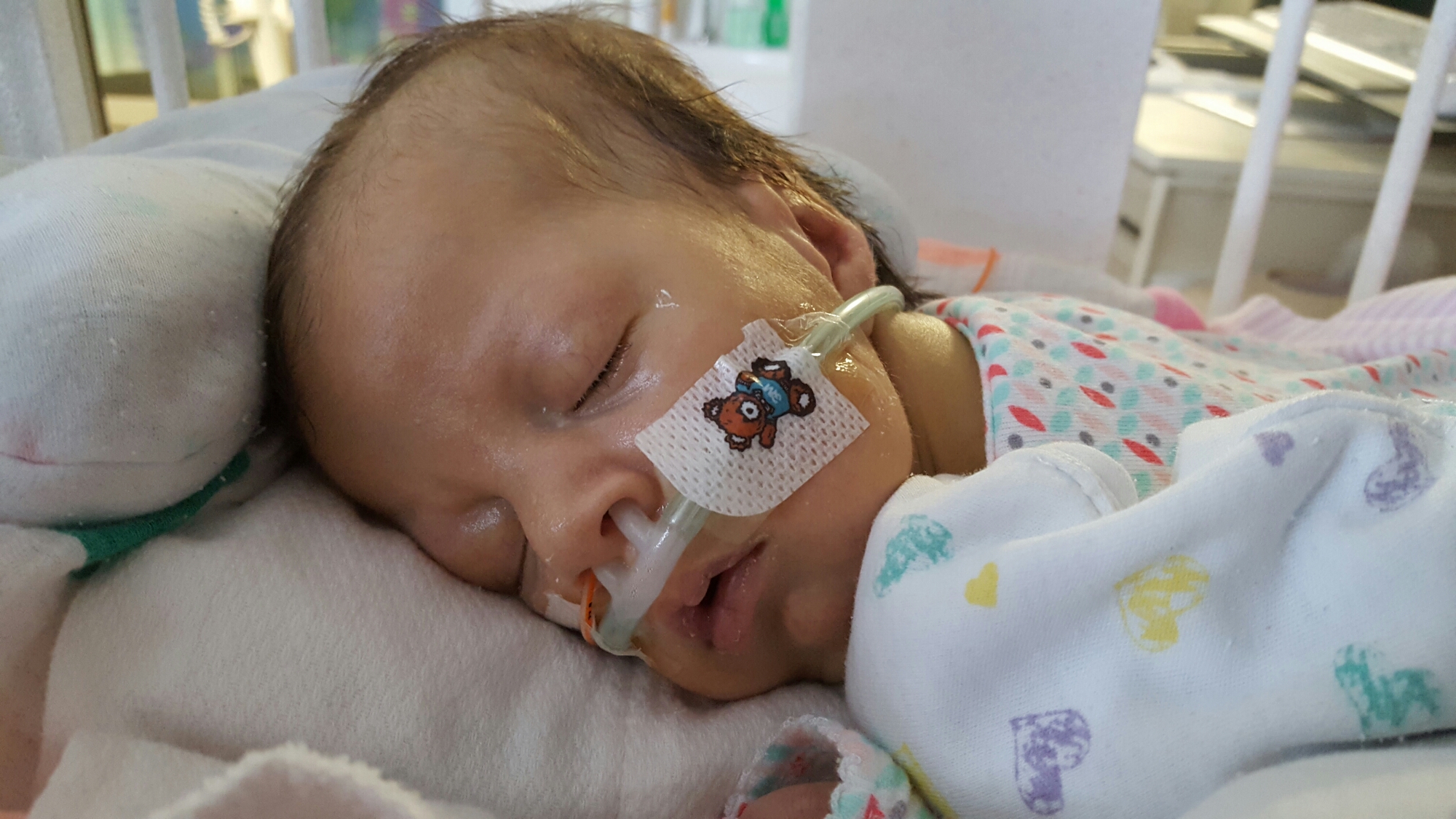
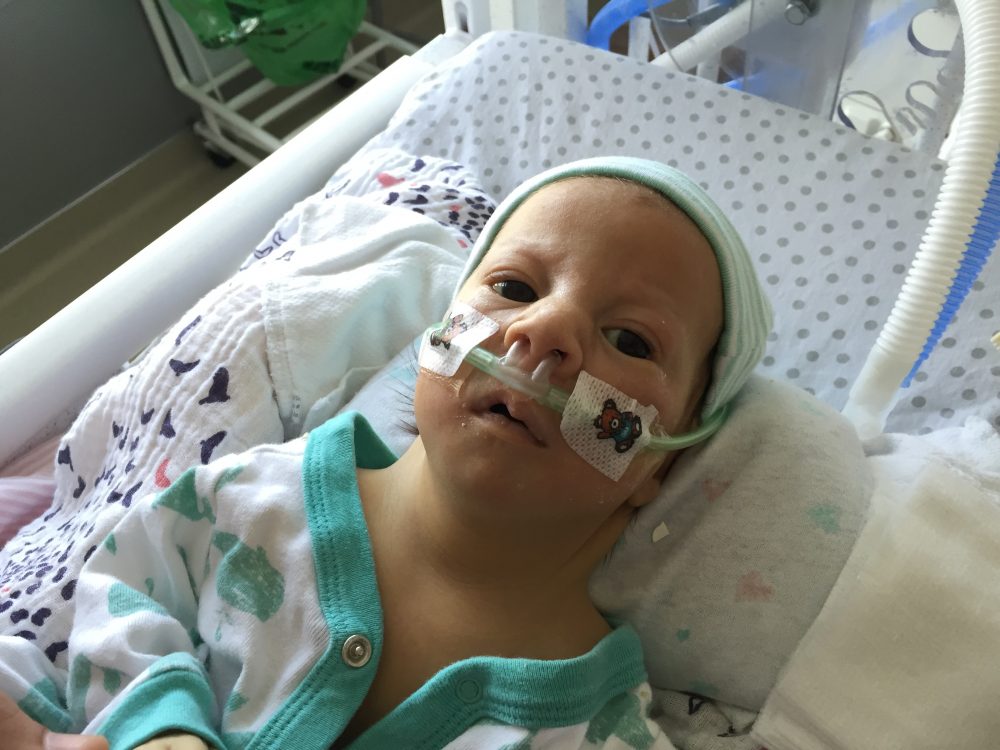
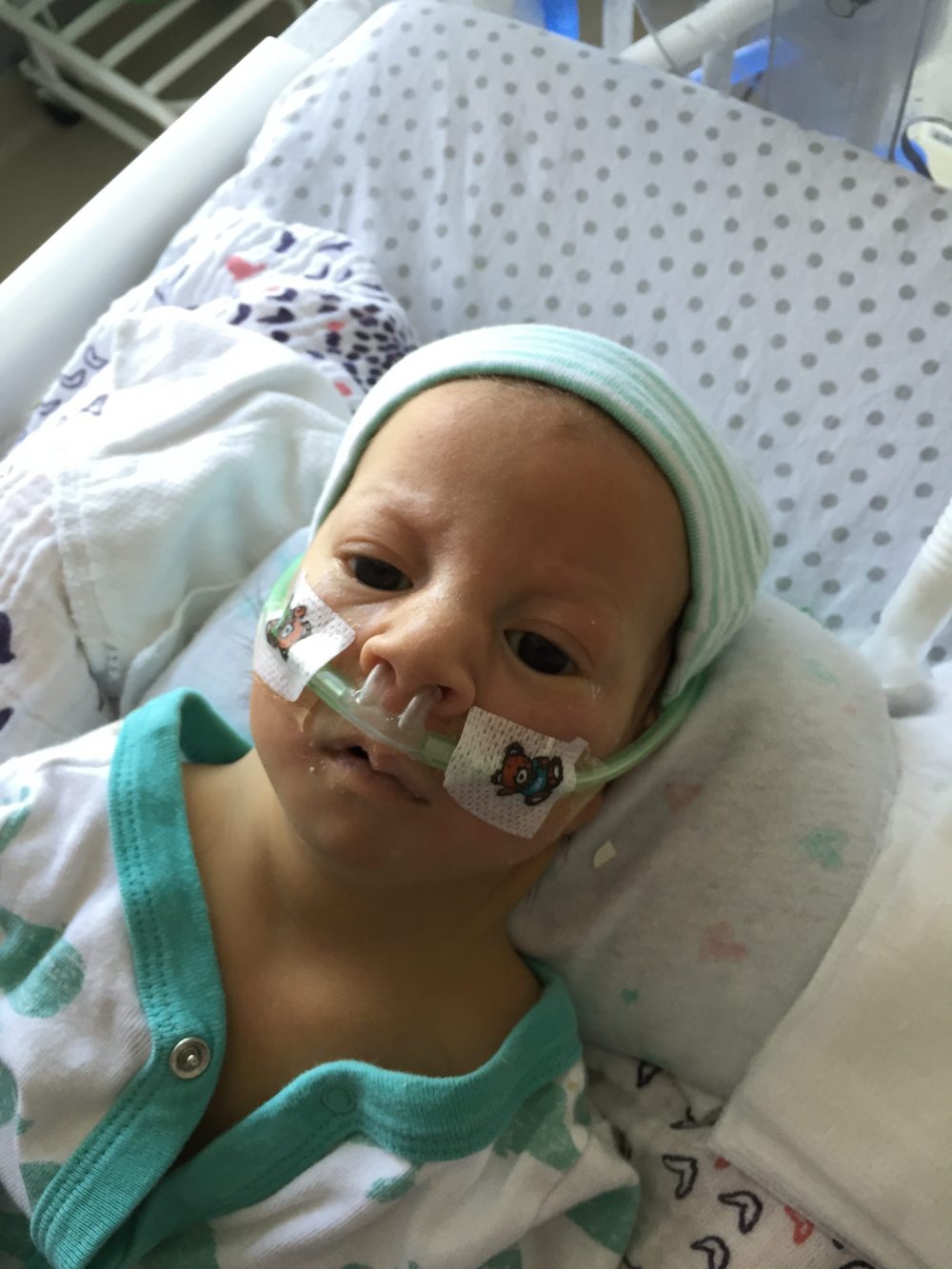
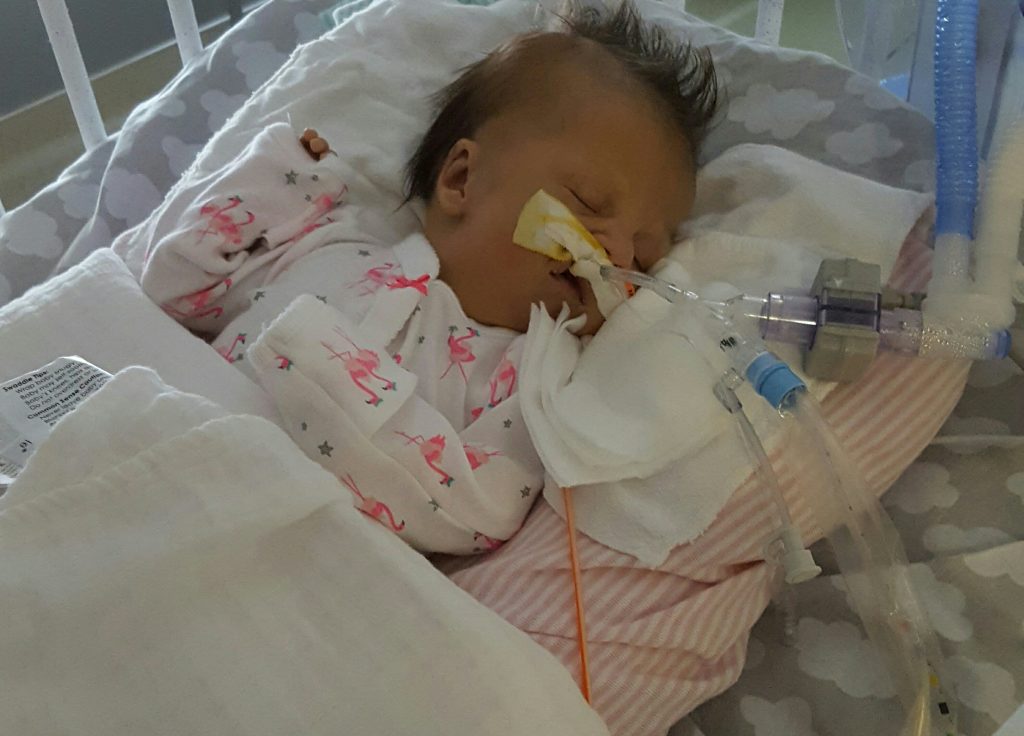
Yesterday we shared the passing of our beloved daughter. Today, we want to share a little bit more behind her story.
On Tuesday, Olivia went for a muscle biopsy. Results from our recent advanced genetic screening found a “variant of unknown significance” in her TTN gene, which is responsible for the Titin protein in our bodies. Mutations on this gene could have easily explained her condition, since the Titin protein plays such an important role in how our muscles function. However, since the science of DNA is still developing and this specific mutation was never before seen, a biopsy was supposed to provide the physical evidence needed to confirm that mutation was the cause of her condition.
Instead, what we found was Olivia suffered from a rare form of Spinal Muscular Atrophy (SMA). SMA is actually a fairly common genetic diagnosis, but Olivia had what is called the “non-5q” variety. Non-5q refers to the fact that it’s caused by mutations outside of the common SMA-causing genes (chromosome 5, section q). This variety is very rare, hence the inability to diagnose it clinically or with our previous advanced testing. However, once they got a look at her muscle tissue, the diagnosis came in quickly.
The Wikipedia page for SMA is useful, but it doesn’t describe the non-5q branch at all. Her core team gave us this paper in Neurology which provided a helpful summary (going to work on getting a complete copy for here). In short, its prognosis is fatal and the life expectancy of infant onset is even poorer than SMA type 1.
We never confirmed if the TTN gene mutation also impacted Olivia. Her tissue sample was too atrophied by SMA to be conclusive. Also, systematically speaking, nerve firing causes muscle movement, so whether her muscles were healthy or unhealthy (from a TTN mutation) without SMA, didn’t matter much for the prognosis, because SMA affects the nerves leading from the spine to muscles. Our Titin explorations were looking at issues with the proteins forming the muscles directly, but in this case, they weren’t getting the full signals from the brain due to SMA.
Despite all this, we still have one test pending. While we know she had SMA and we know it’s non-5q, we don’t yet know what gene caused it and how/if it was inherited. To help us figure this out and also help our family planning all three of us had blood drawn on Friday for a whole exome sequence. Results will take a few months to be processed. We hope this data will also help future cases of her disease be diagnosed faster too.
In the end, while devastated with her prognosis, we were relieved to have a concrete diagnosis. Her case riddled so many medical professionals and labs that we worried we might be forever stuck with unanswered questions. As Dr. P said to us, her final gift to us was to let us know what she needed. She did that and she’s still a pink zebra.