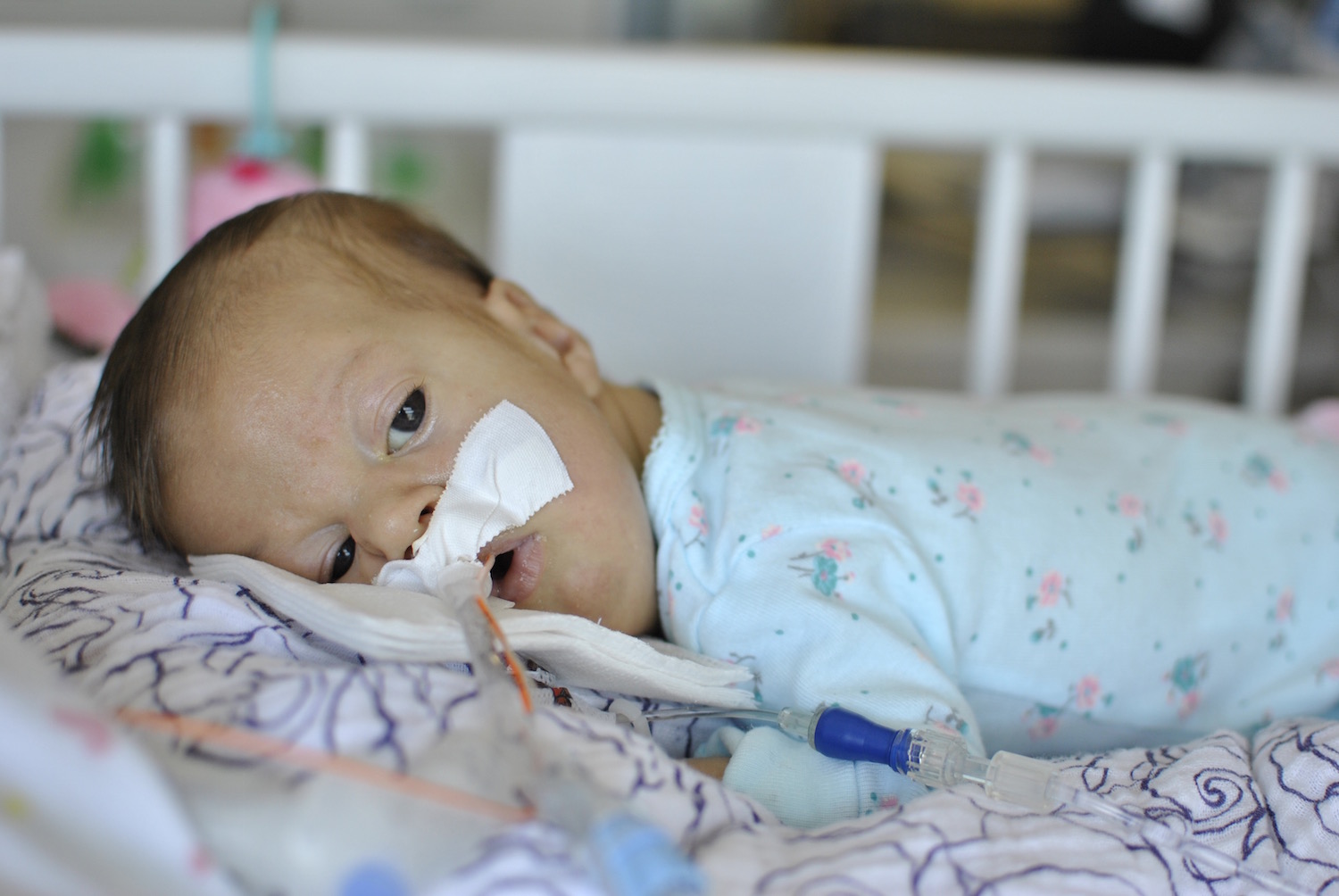
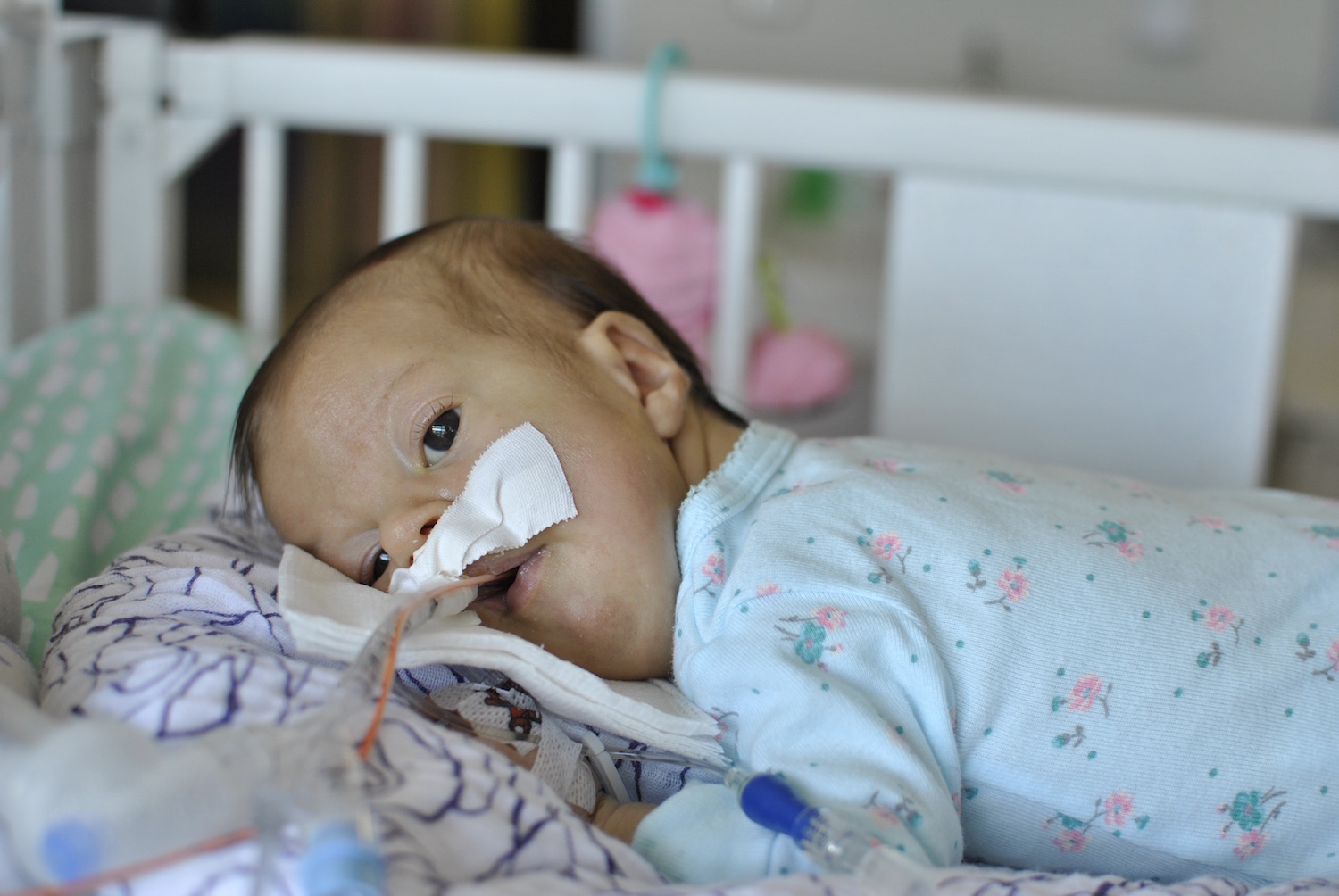
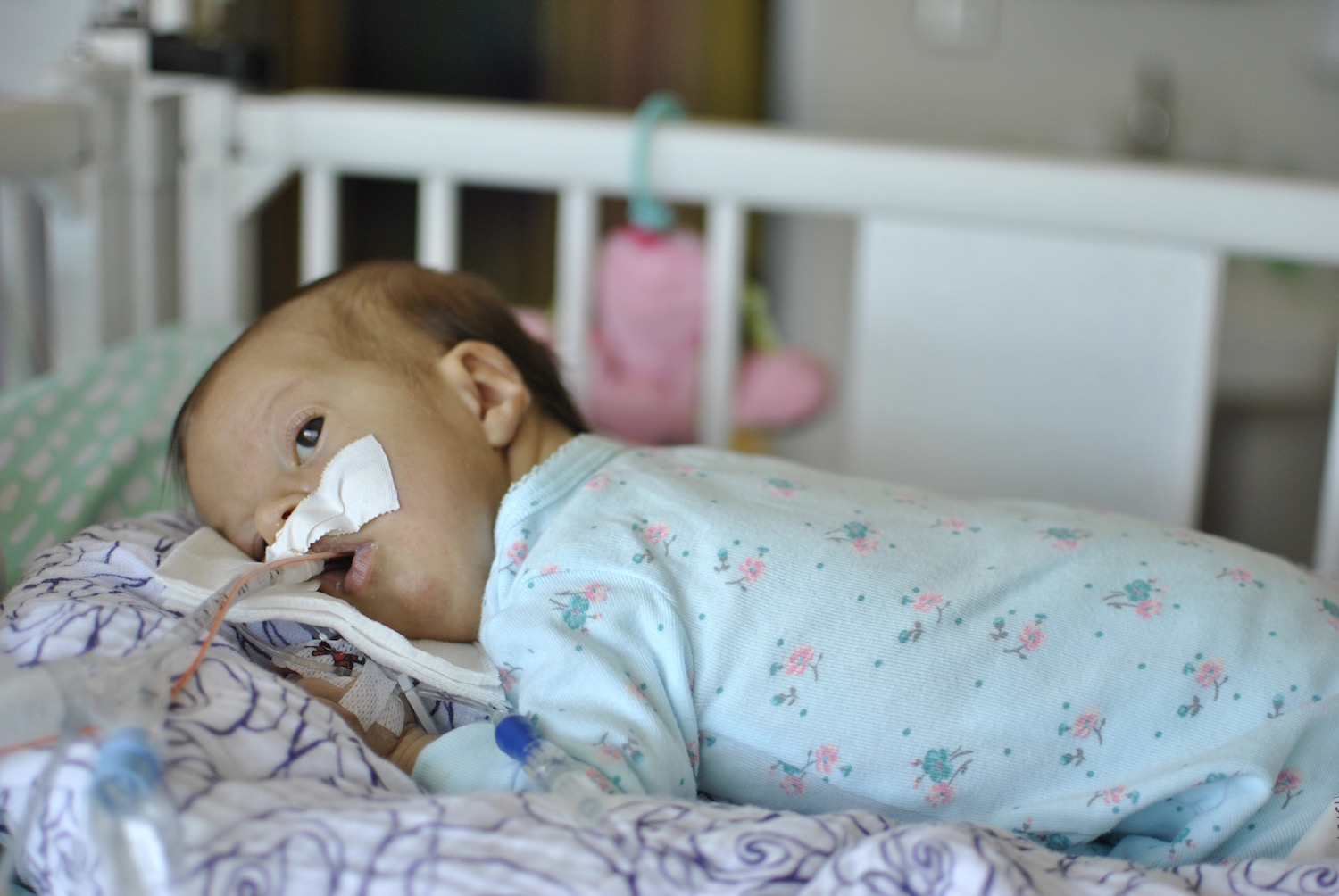
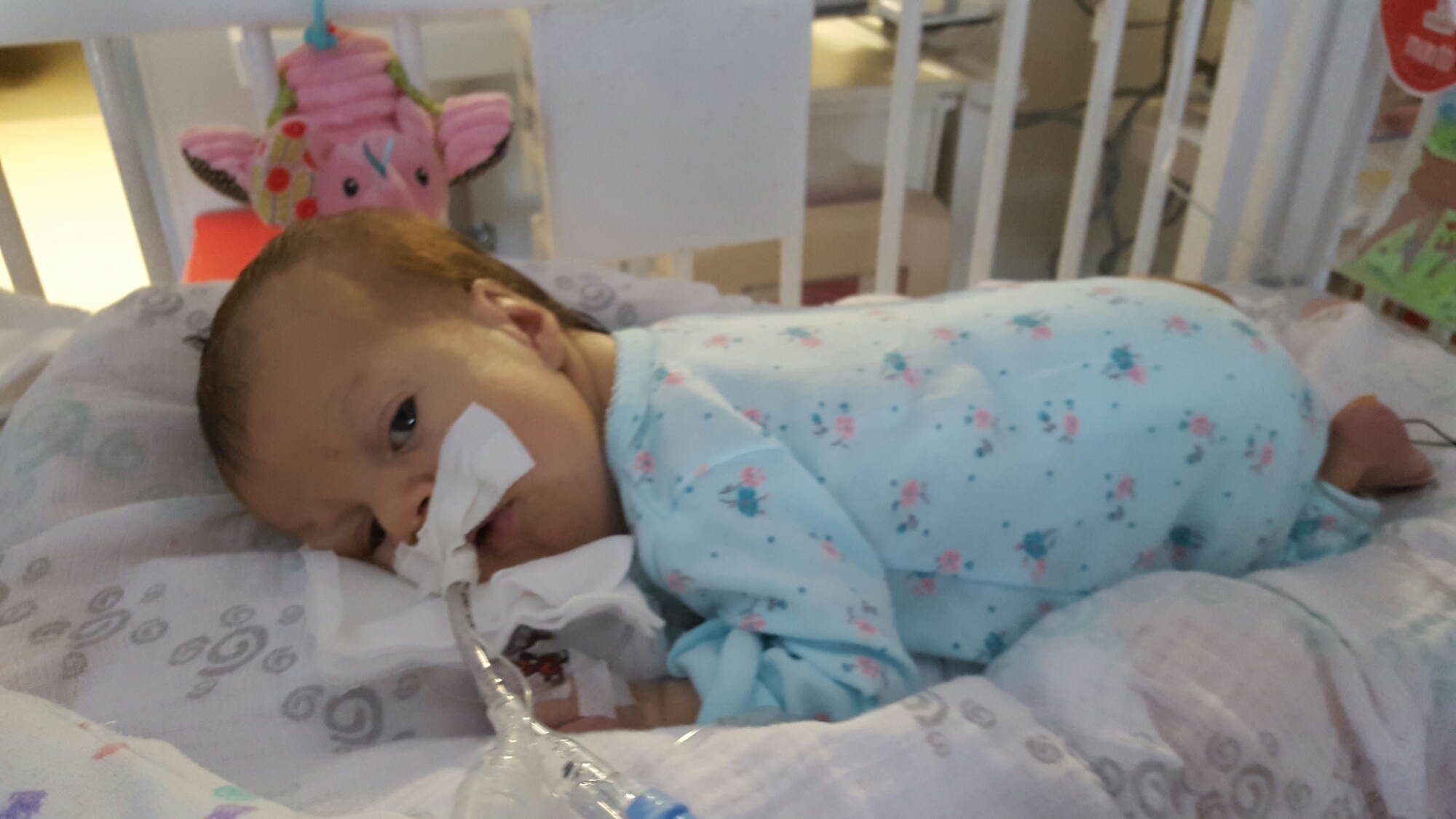
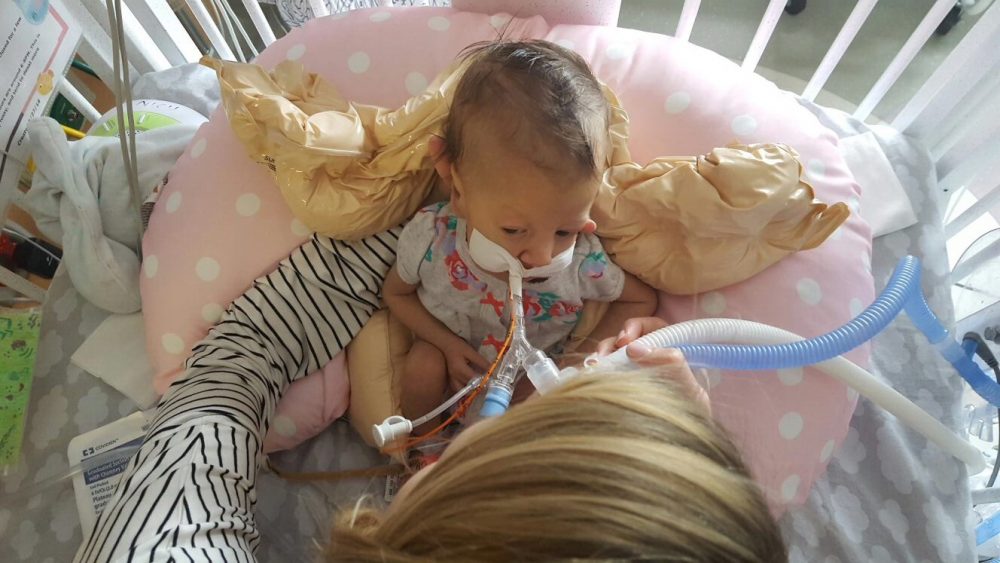
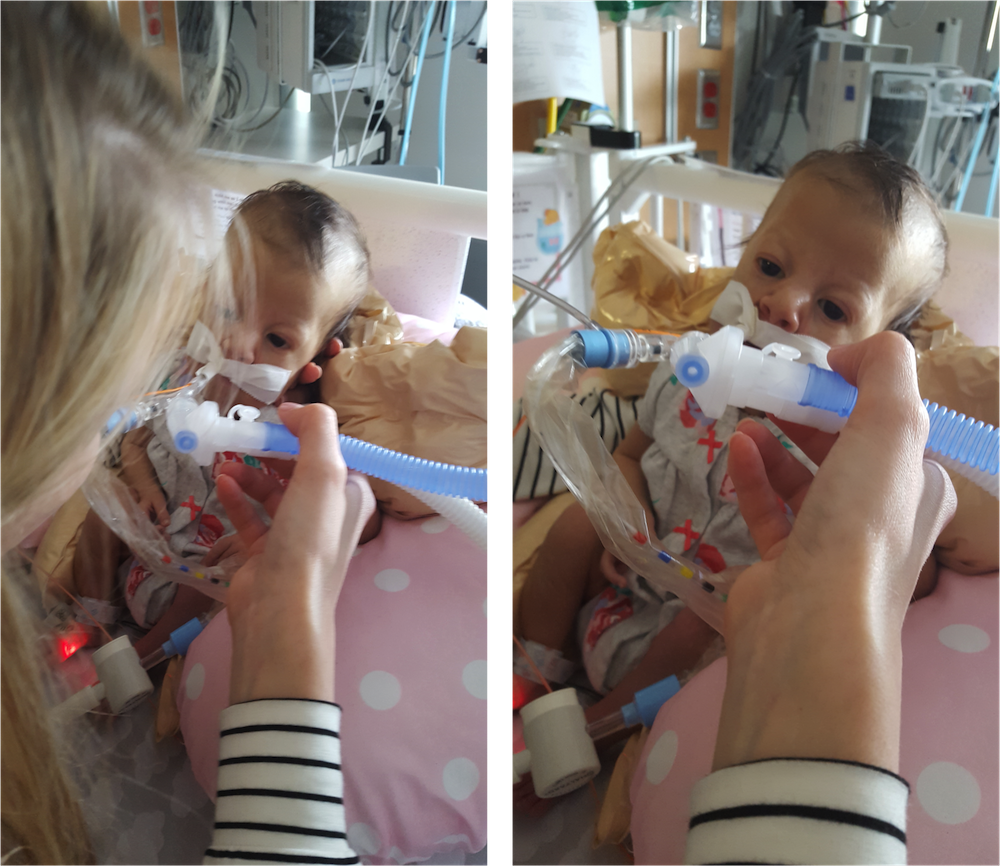
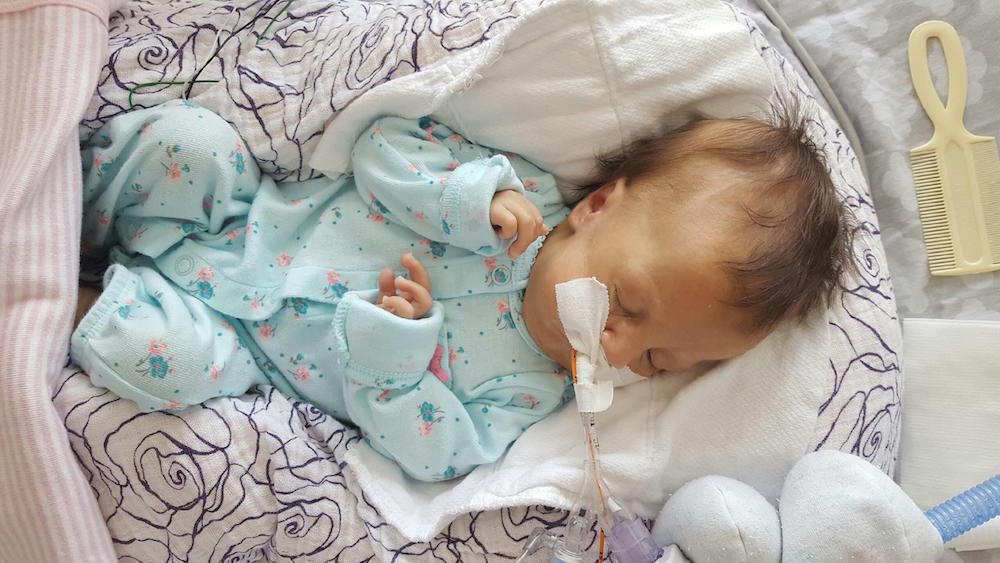
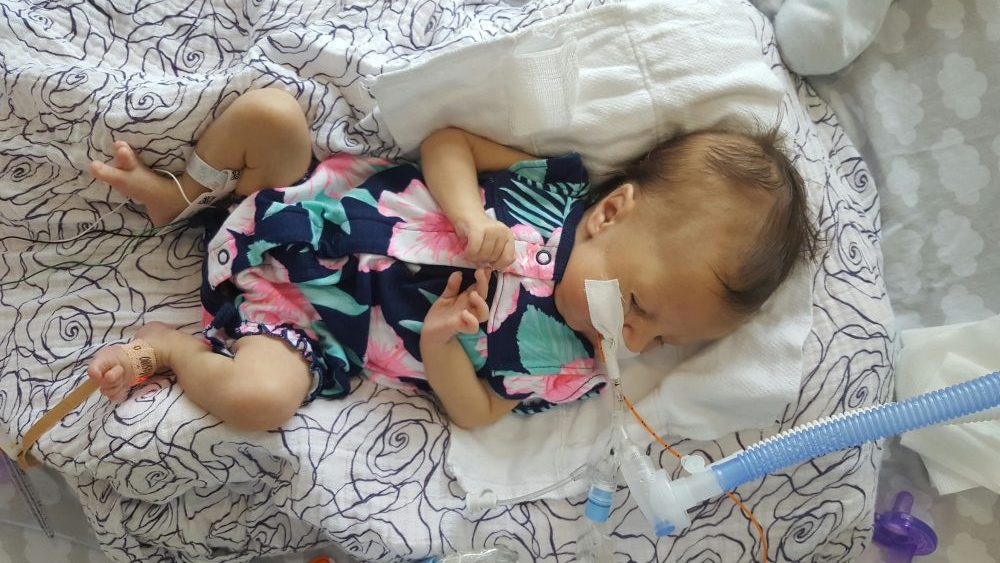
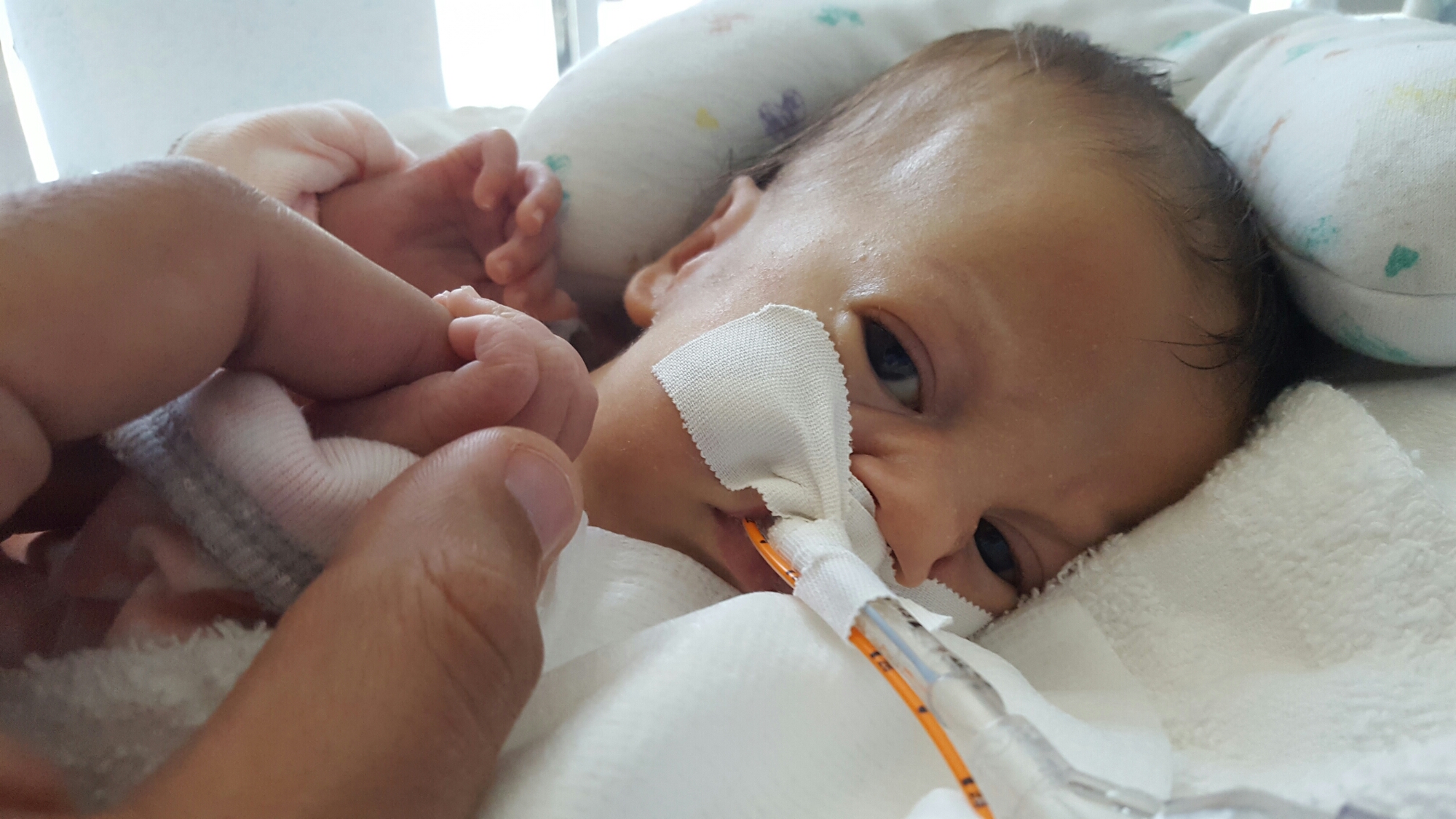
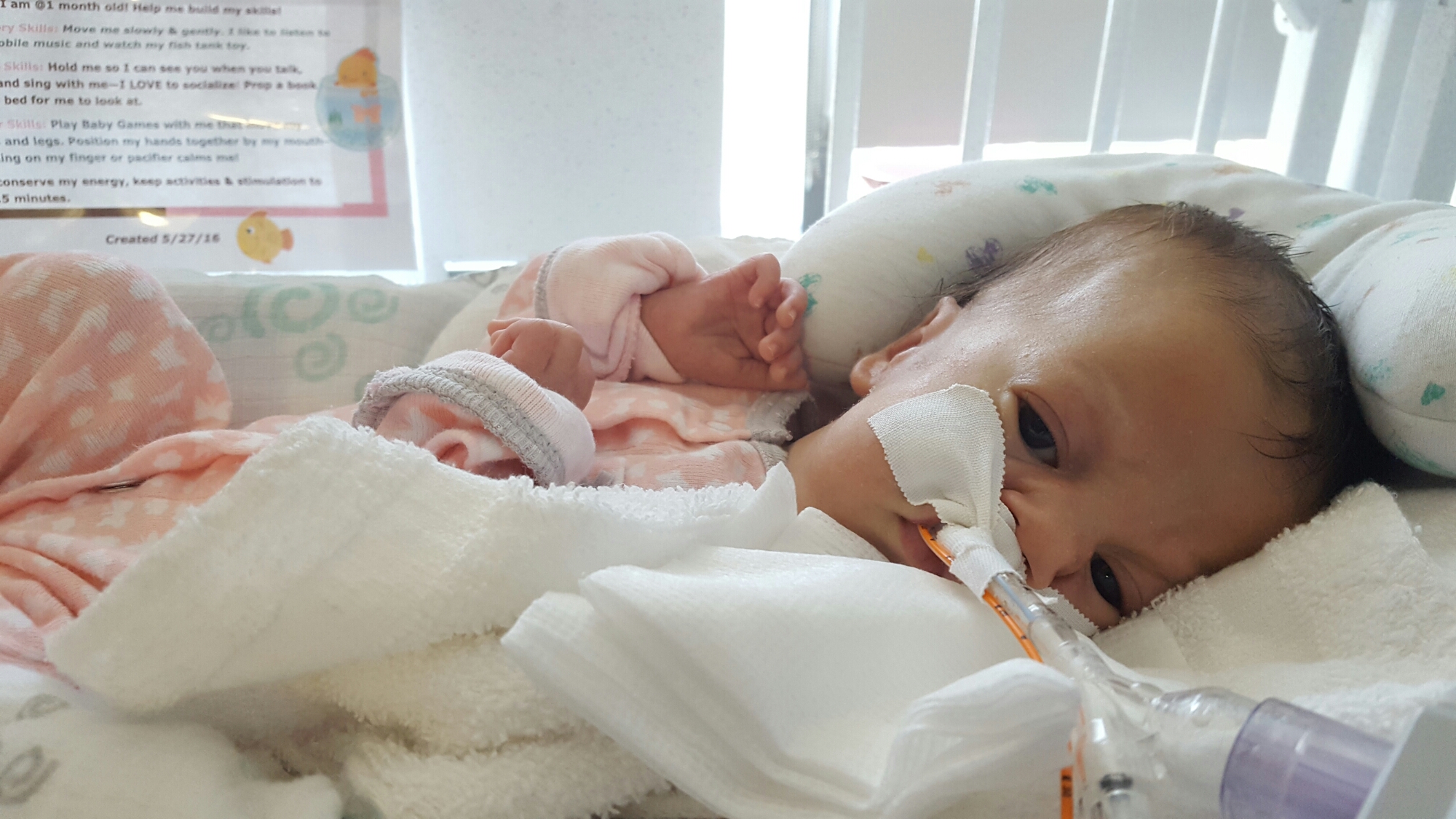
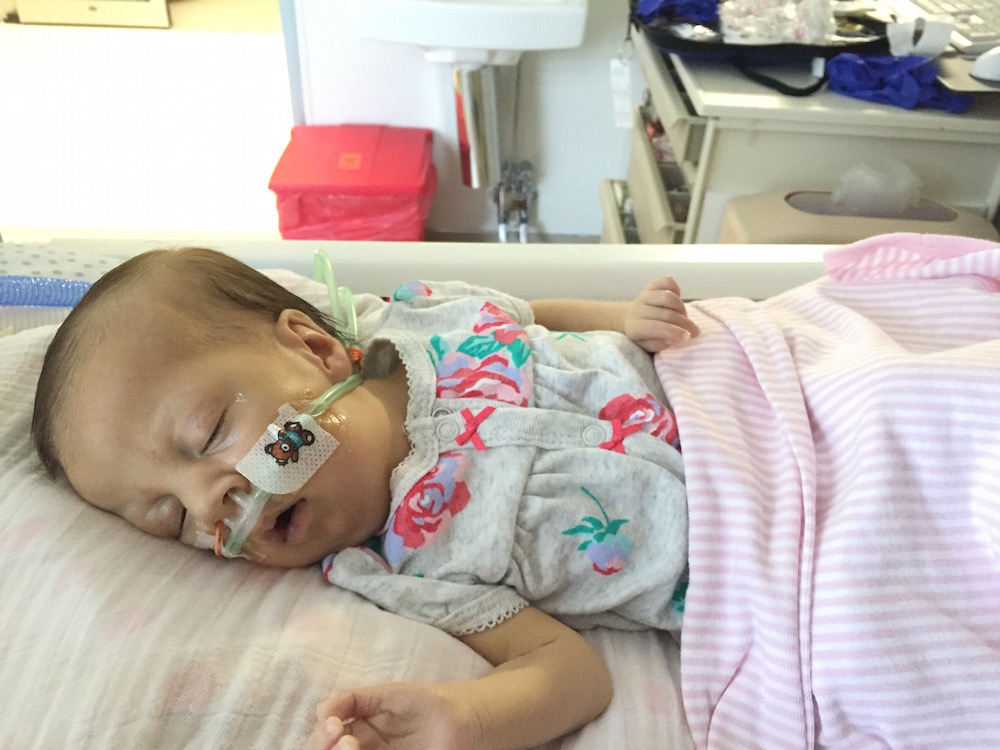
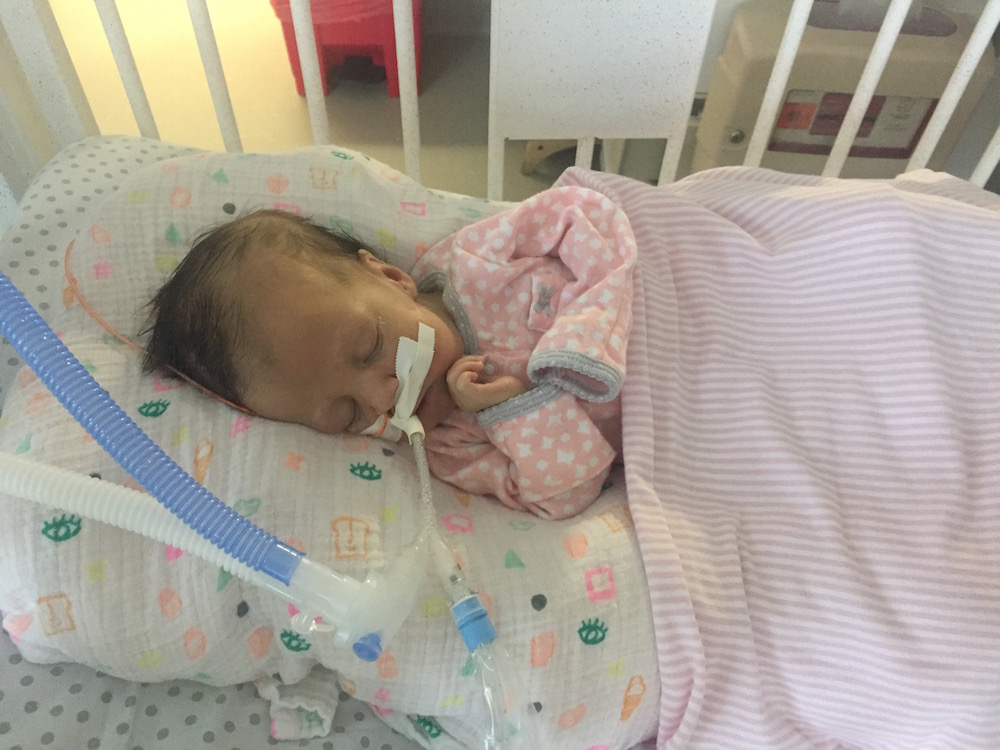
Late one night, sometime shortly after Olivia was born, one of my oldest and dearest friends called, planning to leave me a supportive voicemail. I surprised her, by picking up the phone. We spoke for quite awhile. I shared with her more details about Olivia’s status, her condition, my emotions, than I had with anyone else. See… she’s one of my oldest friends, she’s incredibly straight forward… and she’s a nurse. Not only is she a nurse, but she’s a nurse in an intensive care unit. The words surgical and trauma are in there somewhere too. Maybe in a different state – with adults, not neonates – but regardless, she’s a STICU nurse so she sees a lot of crazy, messed up shit on the regular.
She said a lot that night, but one of the more simple, sticking points was: we have to be prepared for good days and bad days.
Maybe a lot of good days followed by a couple of bad days. Maybe some bad days followed by just one, glorious, good day. But that it was going to be a journey. An up and down, and up and down, and up and down kind of journey. We had to be prepared for a journey that may not be a simple and steady rise of good, better, best days.
This week has been a week of more bad days than good.
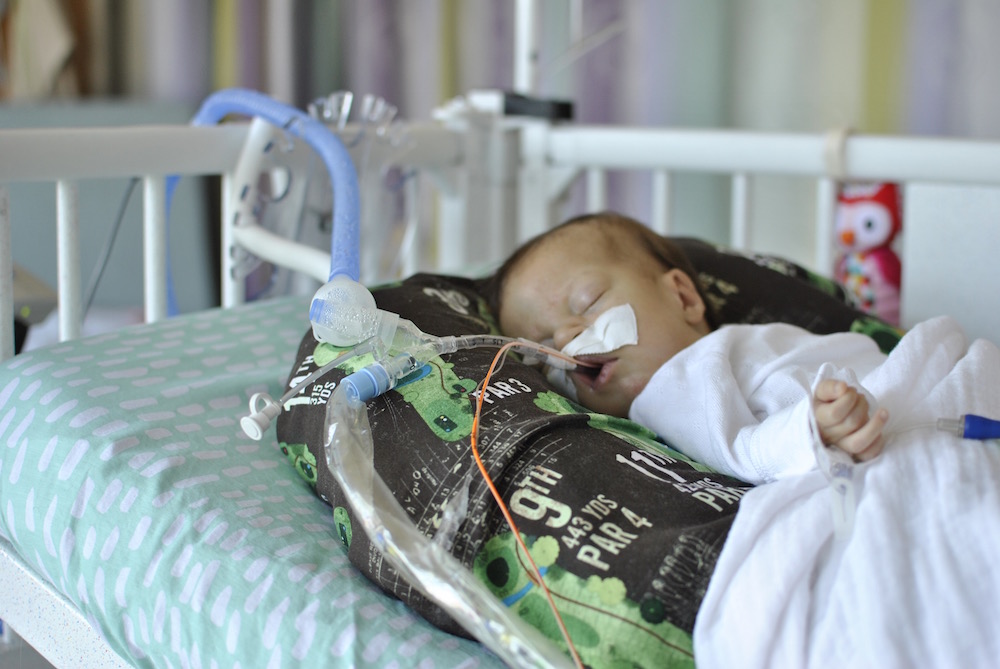
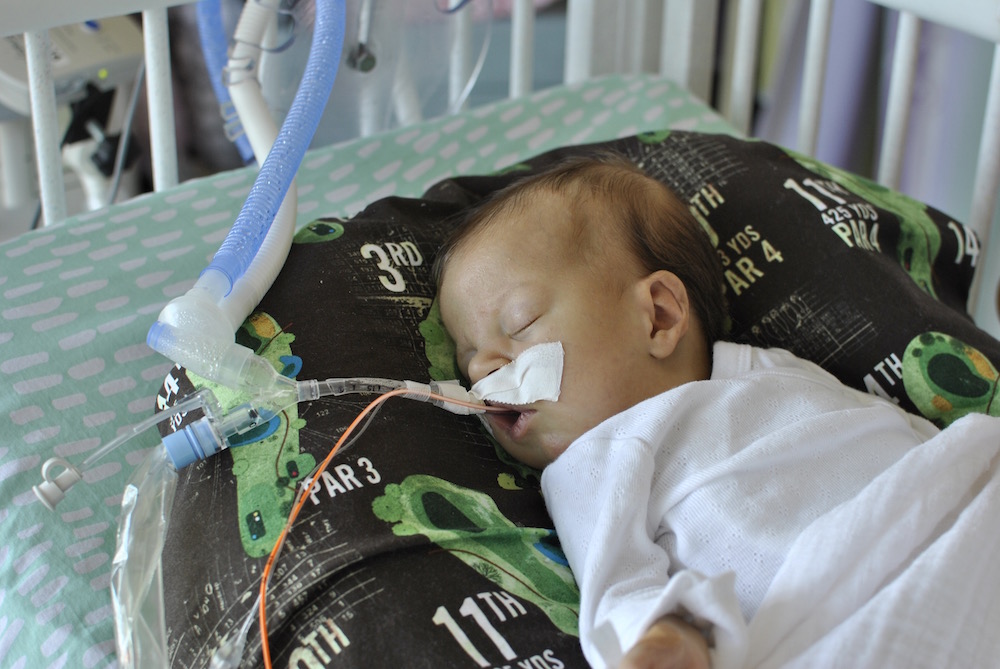
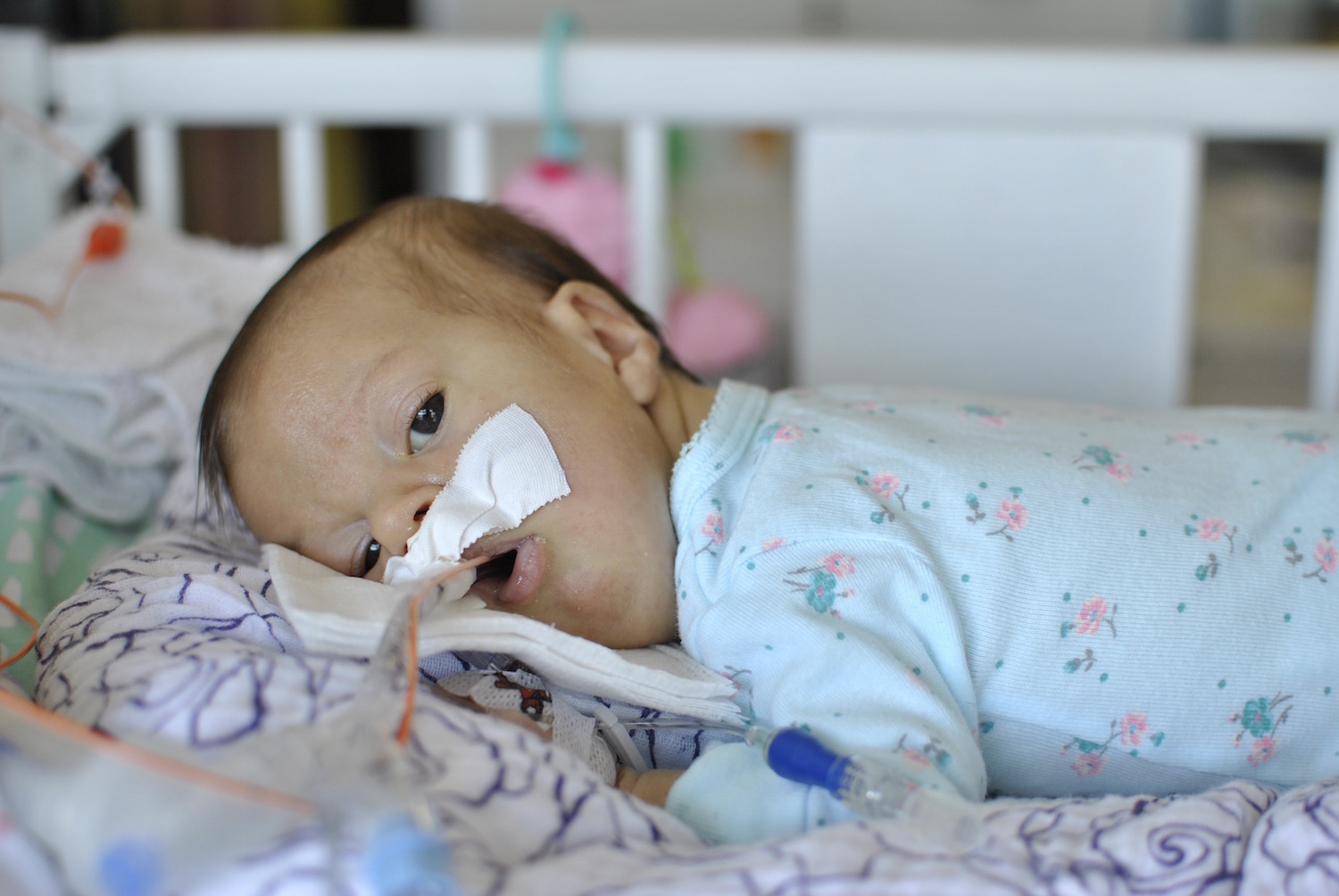
The respiratory events have continued each day since Monday. She’s thankfully been sleeping well (and uneventfully) each night, but each day seems to be filled with desats, bradys, bagging, and just an overall uncomfortable little girl. We’ve had a series of x-rays, adjusted ventilator settings, continued our usual tricks of rigorous chest PT, suctioning, and careful positioning, and even changed her ET tube to one with a cuff in an attempt to remove her major air leak from the list of possible culprits.
This morning’s xray looked good: no signs of atelectasis and the tube was positioned well. So next up we’re running a whole slew of labs and blood work to rule out infection. In addition, we’re going to begin giving her some fluids since we’ve paused her feeds, we may start her on antibiotics for 48 hours, and we’re reverting back to her original Reglan dosage (since that was one medical detail that had changed this week).
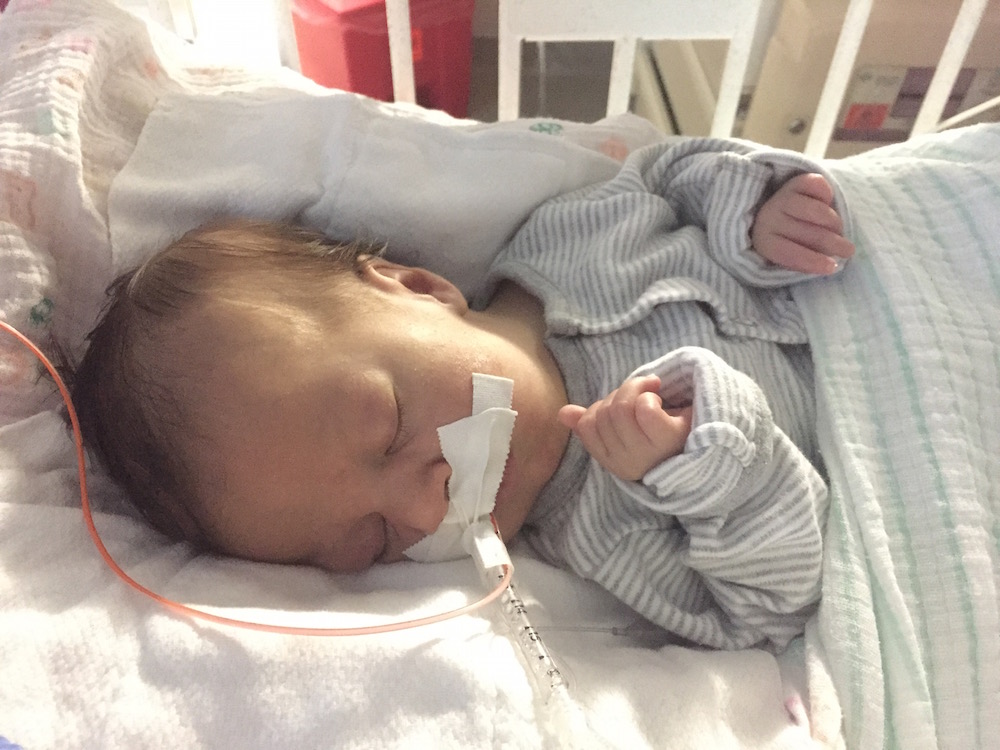
In other baby news: Olivia had a massive blow out all over my favorite outfit of hers, and I successfully clipped all 10 fingernails without any issues or accidents 🙂 Grandma and Grandpa Guerrero will be arriving tomorrow for a visit, and Olivia is working on some special gifts to give Dad on Sunday!