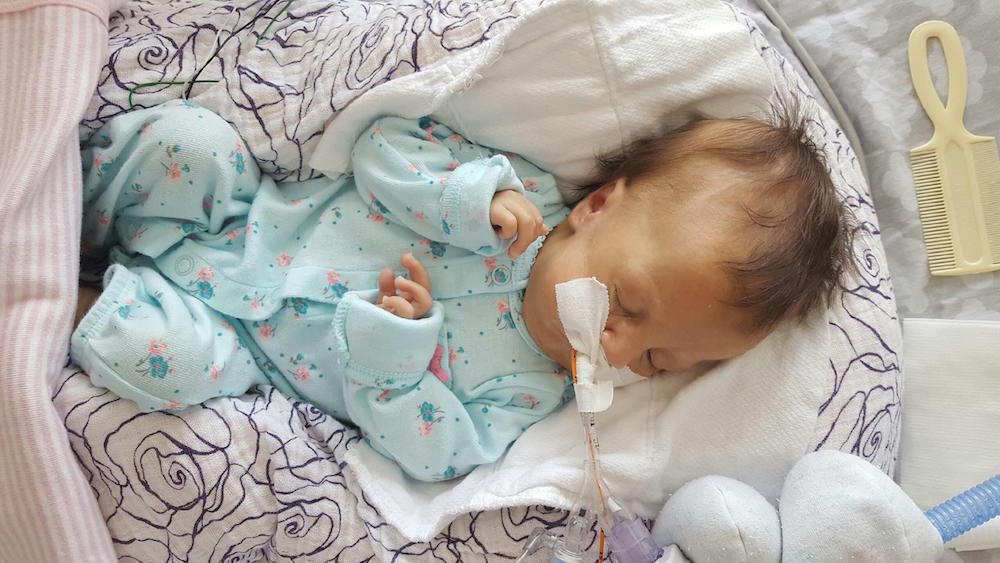
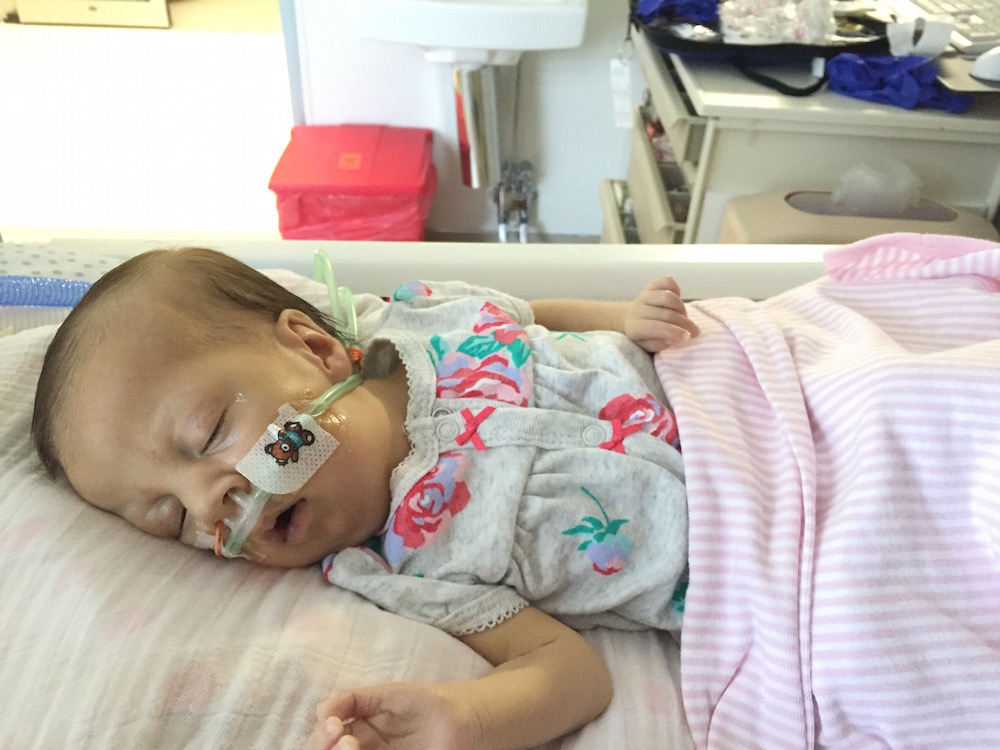
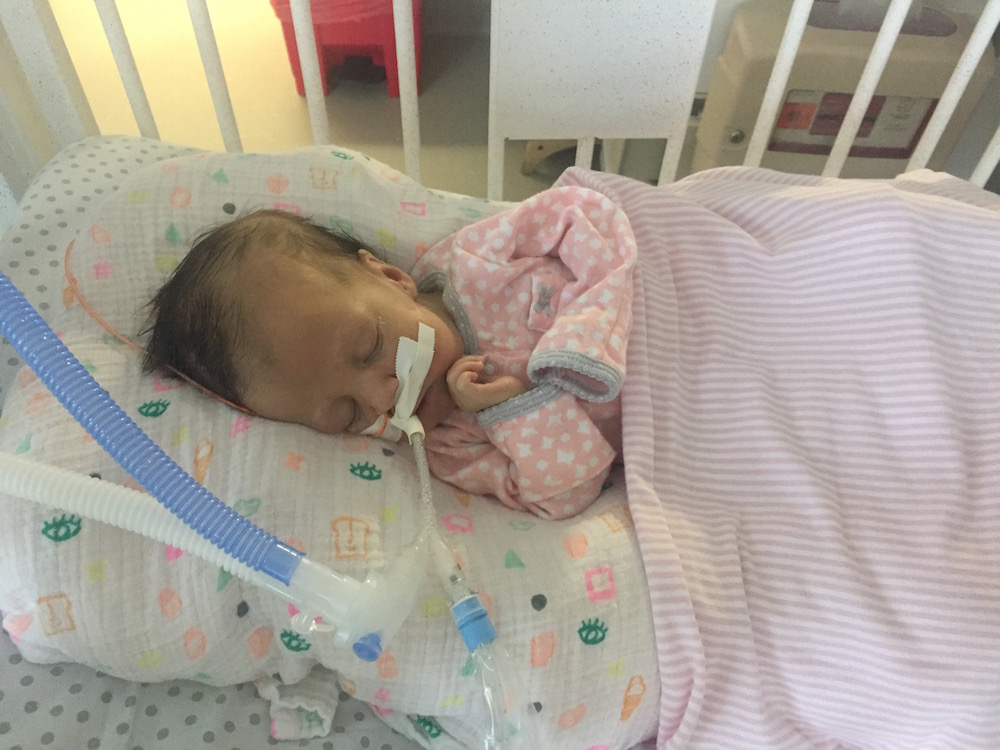
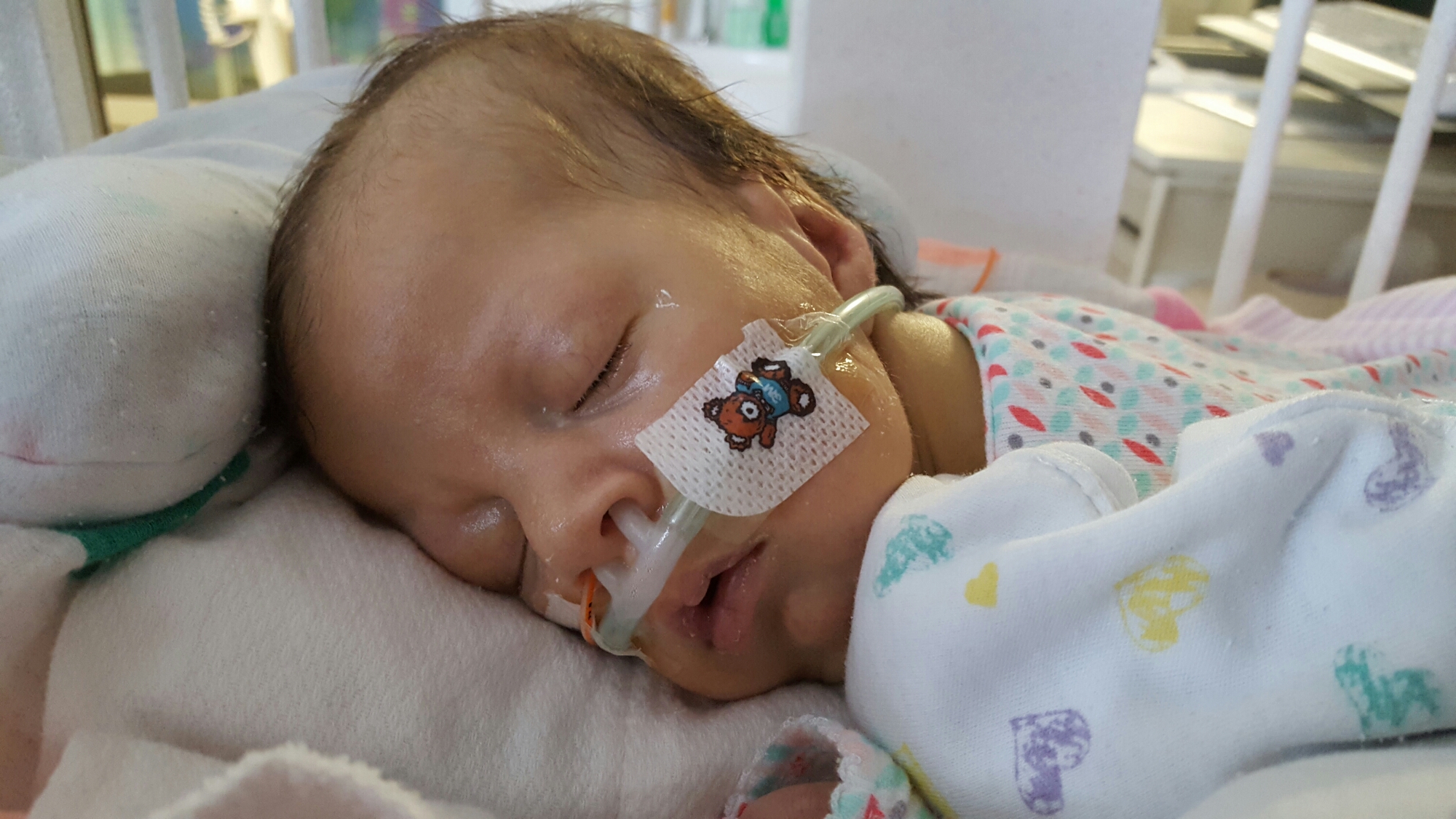
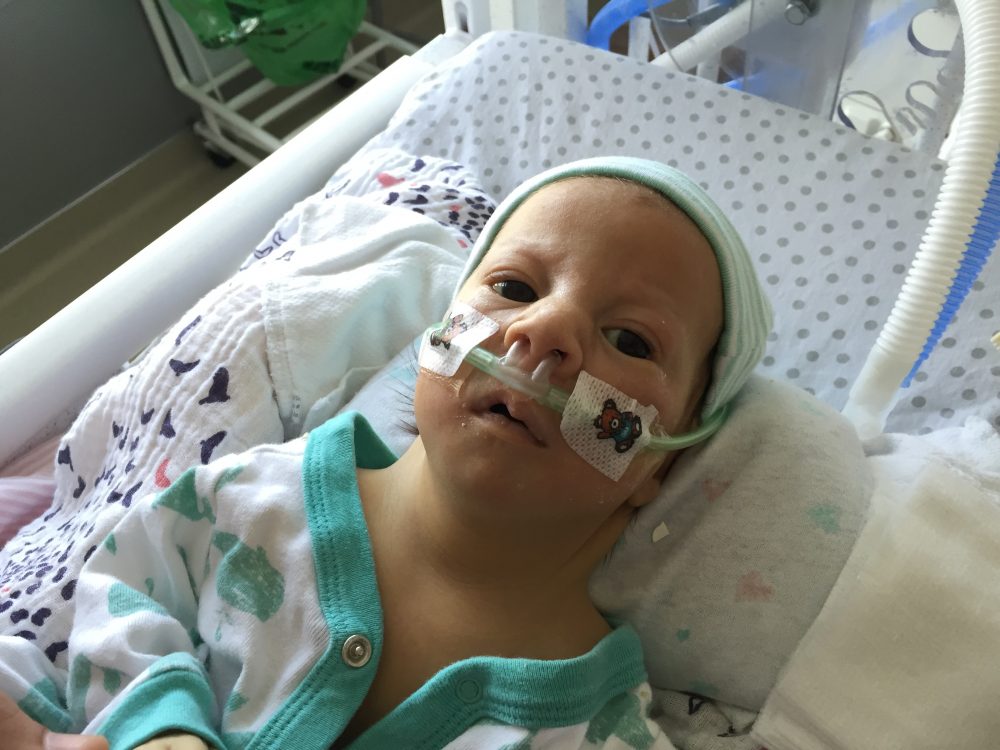
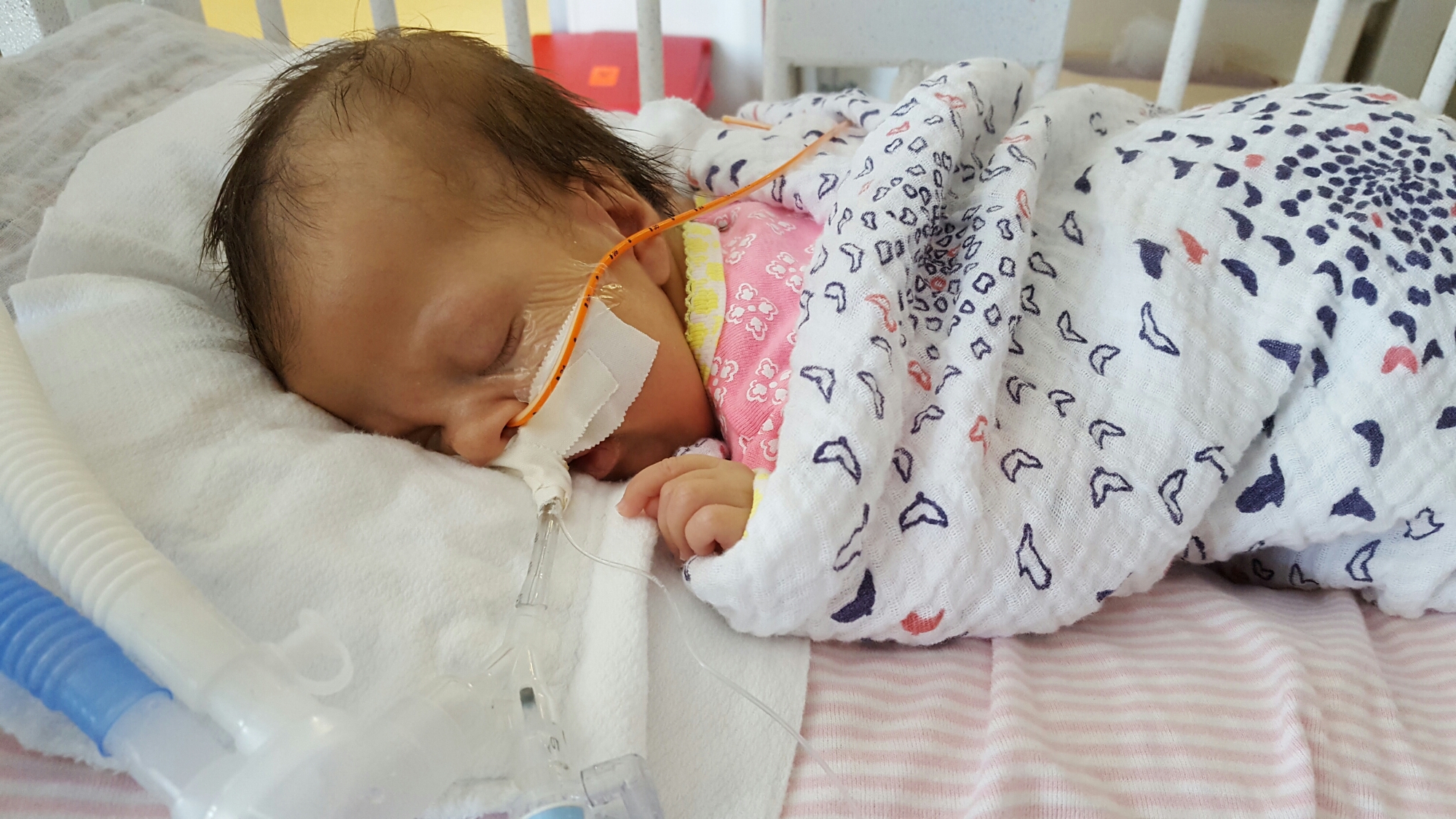
Quiet days continue in room 15.
Nana and Grandpa Prior visited yesterday before heading back to Maine, and Luke and I spent the day and evening with Olivia, per our usual routine.
Most often now a days Luke will arrive first thing in the morning – usually before 8AM and spend the early hours one on one with Olivia. This gives me some quiet time to either sleep in (which I’m quite good at), putz around the house, or run errands. When I head in to the hospital mid morning, we’ll overlap for a few hours, have lunch, and hang out with Olivia together as a family before Luke takes his turn to get outside. Depending on whether it’s the week or weekend, he’ll either go into the office, head home to take care of things like lawn work and house projects, or get outside for a round to relax. It took us over a month before we decided to try this routine, and while we don’t take shifts every day, it’s brought a little bit of balance to our lives, and provides us each some alone time.
Today Olivia has both PT and OT sessions planned, and will likely restart a sprinting regiment this afternoon.
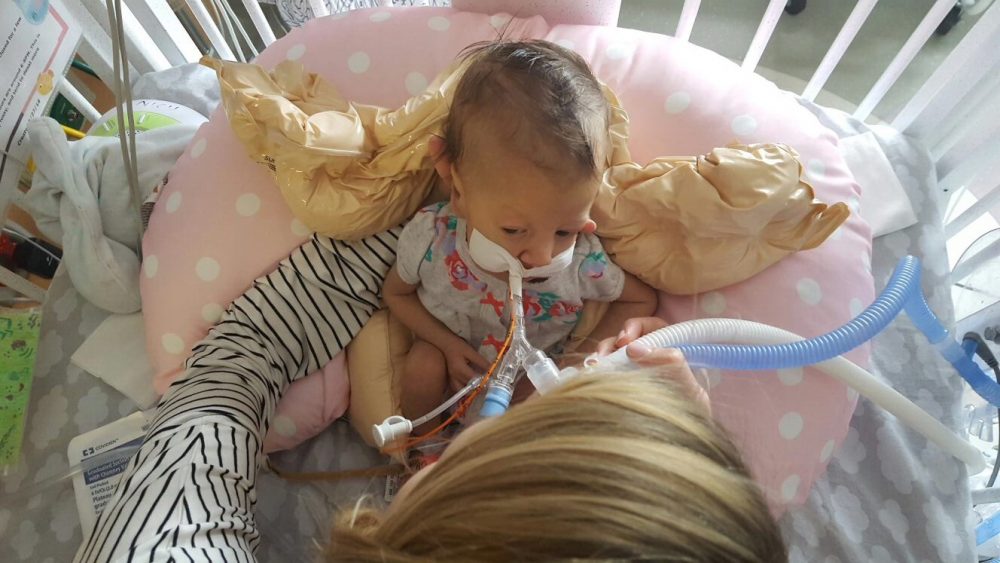
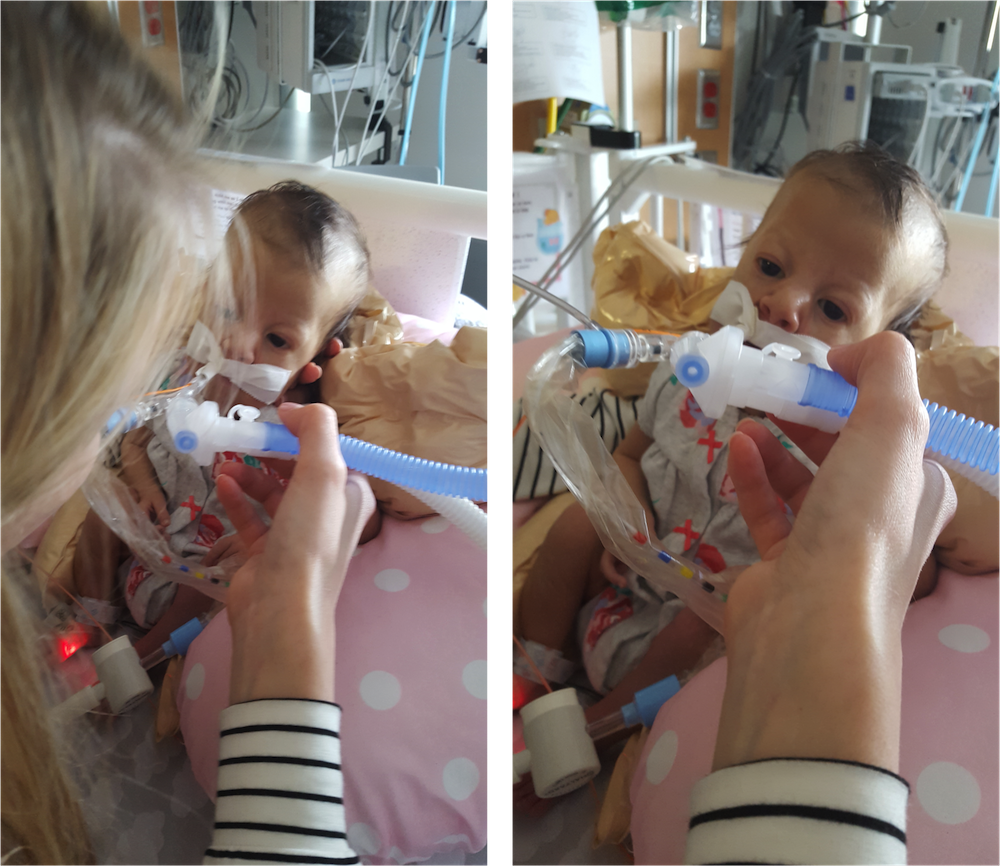
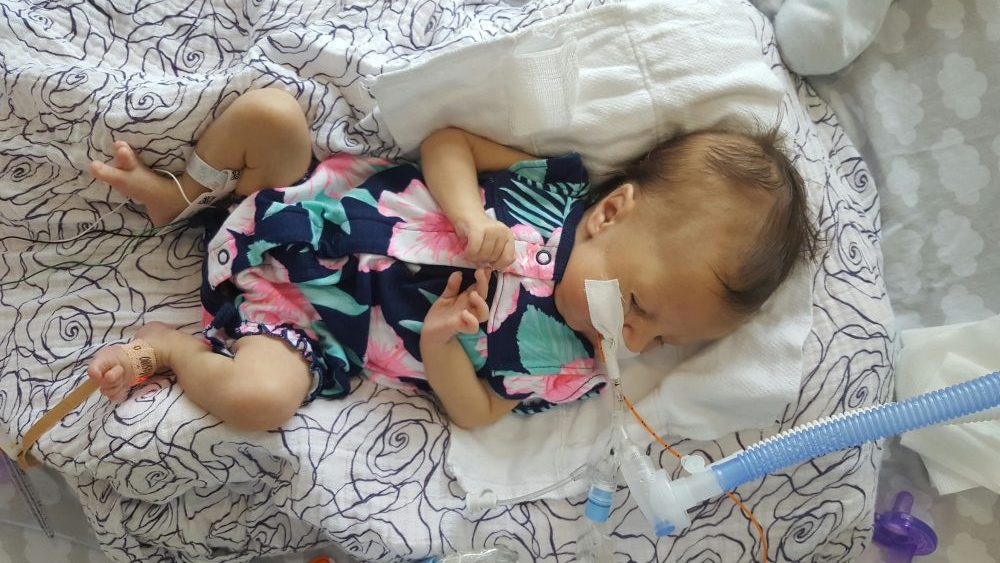
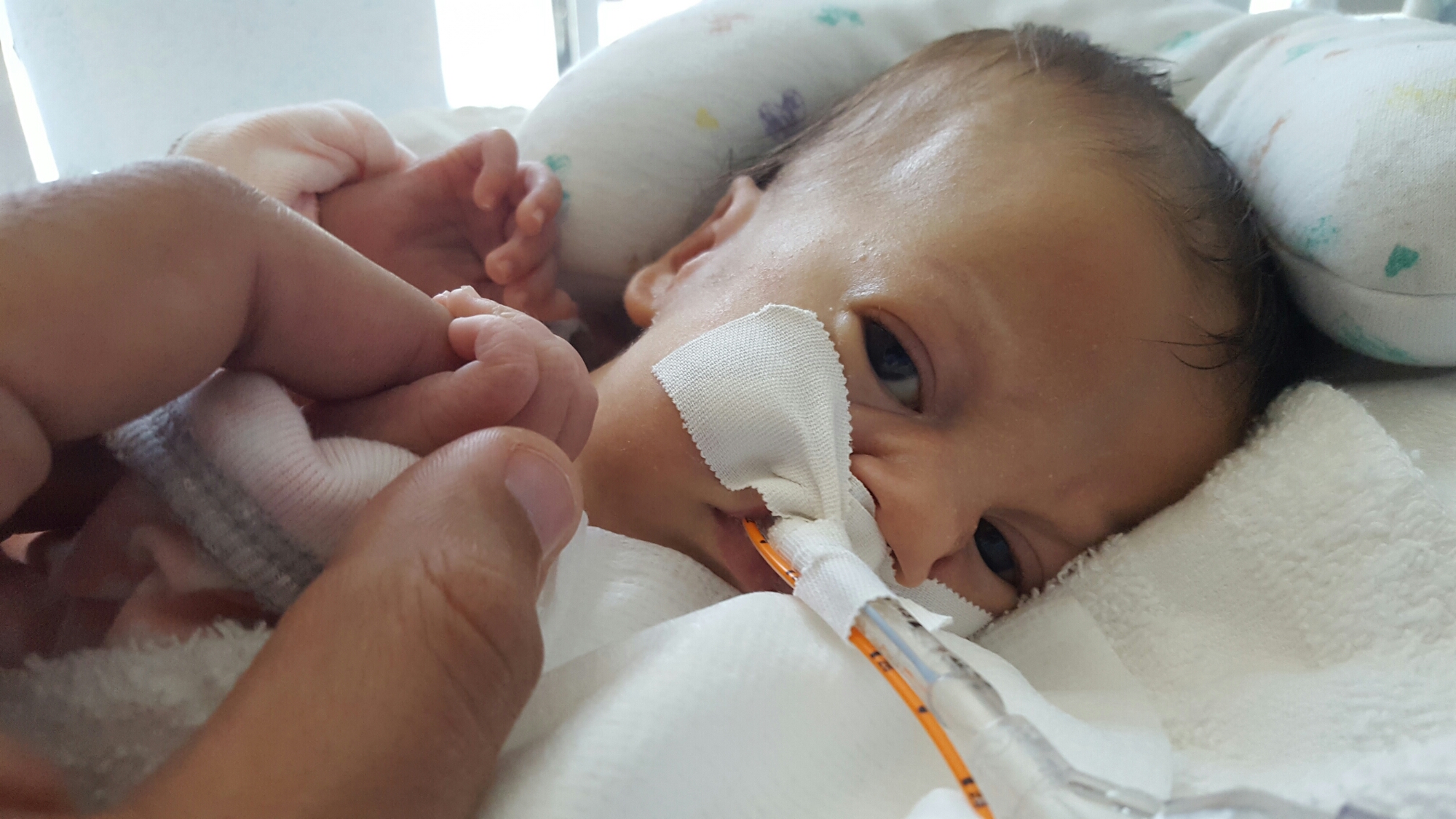
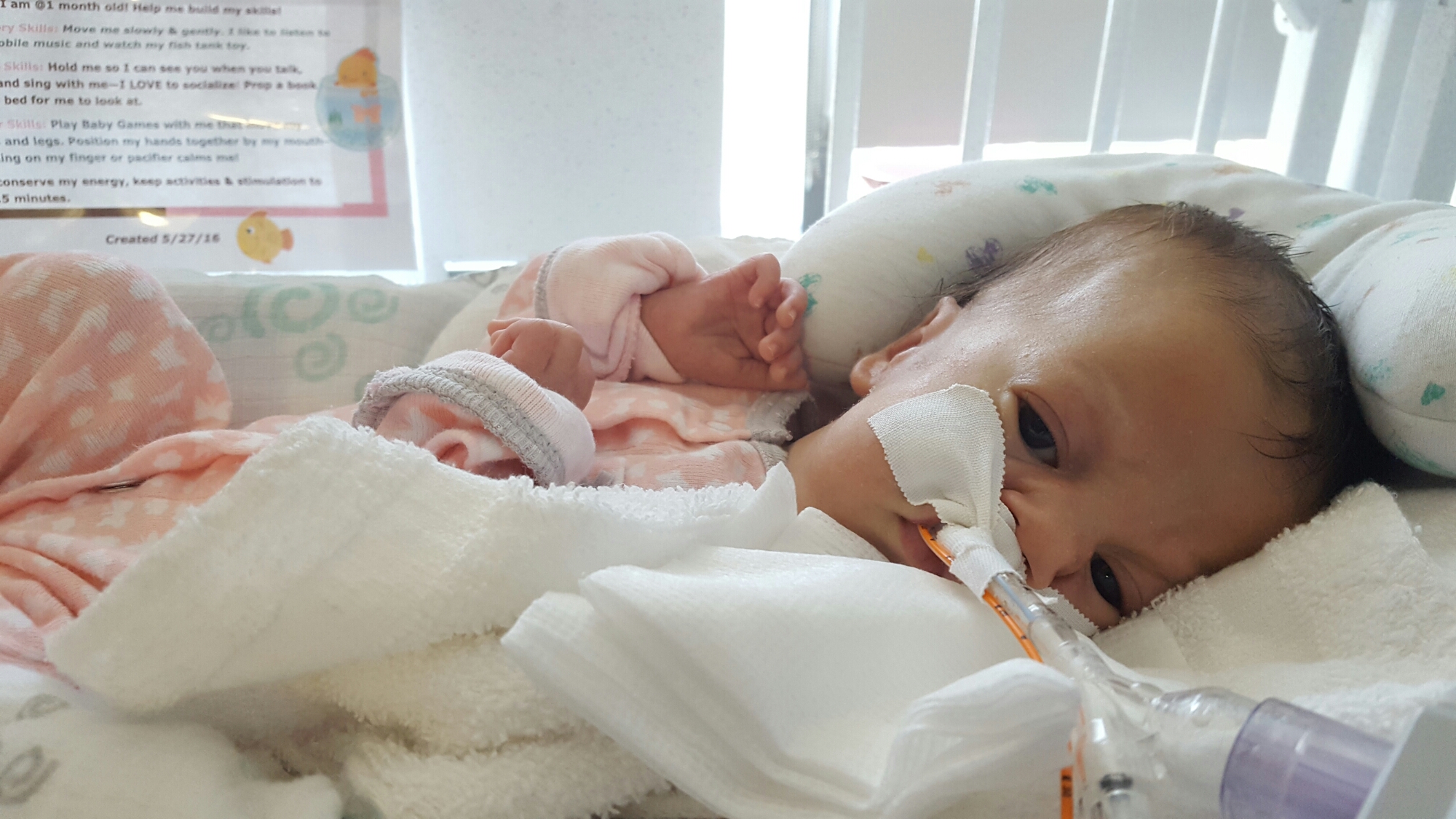
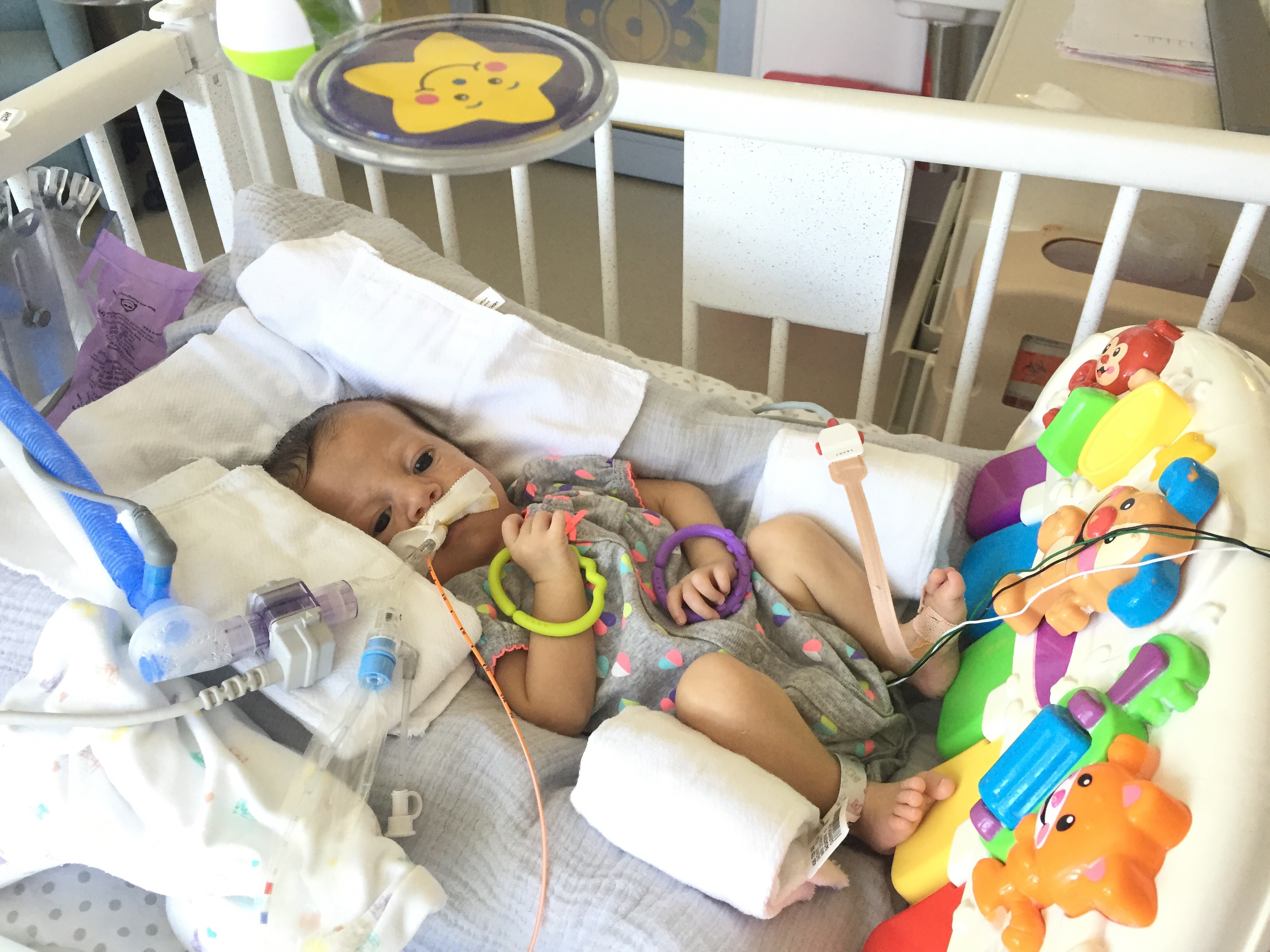
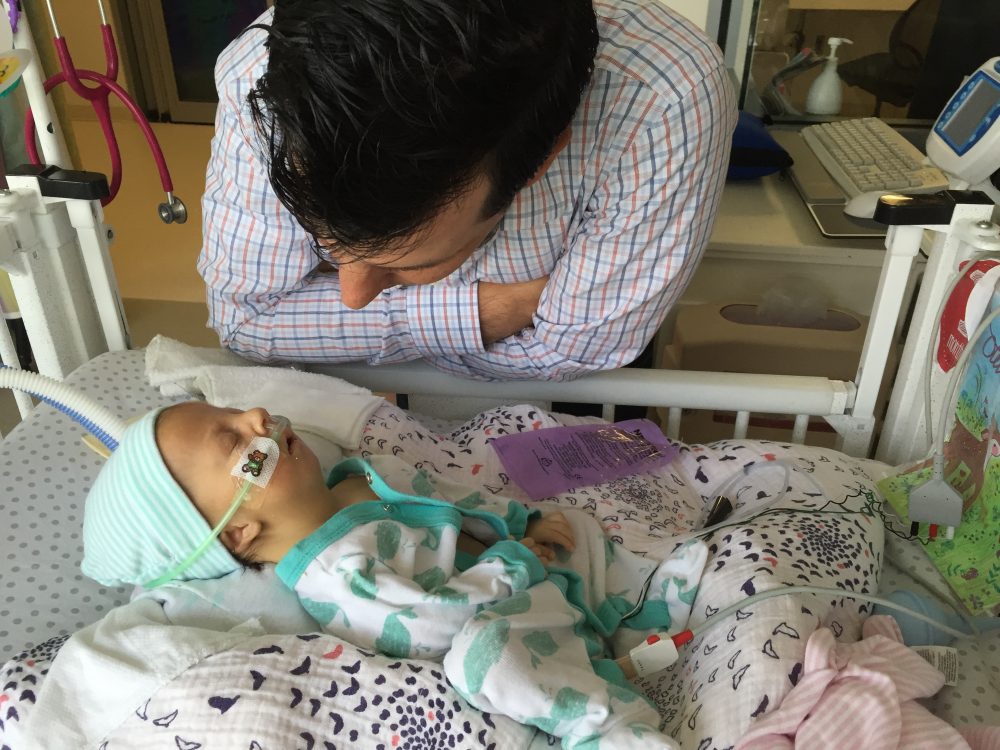
PT and OT continue to work on range of motion and strength, with new fun activities like sitting up! Pictures below show Olivia practicing this new position with mom and dad over the weekend. She doesn’t always “actively participate” – sometimes she likes to relax and let us do all of the work – but on occasion we can feel the smallest bit of engagement from her neck muscles. Steps in the right direction.
Sprinting was discussed this morning as a possibility for this afternoon, depending on today’s weight. The team wanted to wait for today’s weight to see if Olivia was up again from her last weight. Turns out she is up 30 grams from yesterday (now 3030 grams) so we suspect the sprinting will be cleared. While small, the incremental gains day over day are appropriate signs of growth, and hopefully enough to get her back on the growth chart. She was born very small, so we’d be happy to see her back around the 3-5% mark, but ultimately the team would like to see her catch up more and land around the 20-25% range.